Your Questions Answered
We appreciate all the great questions that our readers submit. Here are some answers to common Pulmonary Fibrosis questions we receive.
What is the difference between pulse flow (demand) and continuous flow and when should they be used?
Oxygen can be delivered through a continuous flow regulator. This means that oxygen flows all the time at the same level. When we are breathing, about 1/3 of the breathing cycle is spent inhaling and 2/3 exhaling. In concept this means that all the oxygen that is flowing during our exhalation period is “wasted”. If you have a huge tank or a concentrator that makes oxygen continuously then it may not matter to you. However, if you have a small tank and are outside the house, then conserving the oxygen in the tank becomes important.
The most effective way to conserve oxygen is to use a regulator that delivers a rapid pulse of oxygen every time you start a breath in. The trade-off is that your tank lasts longer but you are not getting quite as much oxygen. As a result of this trade-off, we advise our patients who have a regulator that can switch between continuous flow and pulse (demand) flow to use the pulse/demand flow when they are resting and the continuous flow when they are active and need more oxygen. If you are away from your house and you have a limited supply of tanks then you may need to use the pulse/demand mode to prevent running out of oxygen. Please see the section “Oxygen Used to Treat IPF” for more information on oxygen and IPF.
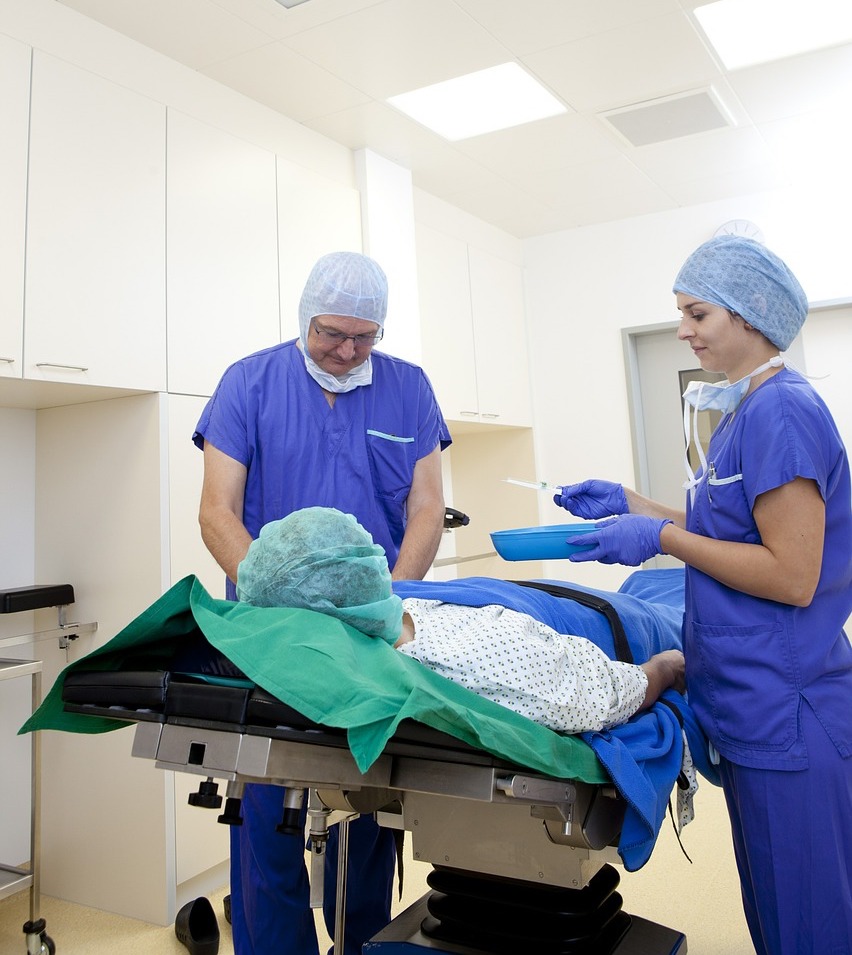
Anesthesia and IPF
We frequently get questions about the safety of undergoing anesthesia procedures for patients with IPF. These are very important questions. The issue is that patients with lung disease are at increased risk of having problems during sedation and anesthesia. The more severe the lung disease – the greater the risk for patients.
These risks include low oxygen levels, the need for emergency intubation, difficulty coming off a ventilator, pneumonia and even death. For patients with mild IPF, we generally allow them to undergo colonoscopy and other procedures provided there is a good reason for the procedure. For patients with advanced IPF, we generally avoid all elective procedures that involve more than mild sedation. We strongly prefer to have an anesthesiologist present to help manage any problems during even minor procedures that involve sedation. Please read our section on preop checklist for IPF for a more detailed discussion.
Are there any genetic tests for familial IPF?
This is a very hot area of clinical research. Many researchers are working to understand the genes involved with IPF. Less than 5% of patients with IPF have familial disease (inherited). These families usually have multiple affected family members as the genes involved appear to be autosomal dominant (a single diseased gene can cause the disease).
There is a commercially available test from Ambry Genetics that can identify mutations in TERT and TERC. These two genes are thought to account for about 10% of familial cases. Genetic sequencing is very expensive and not always covered by insurance. Furthermore, we don’t know that mutations identified in these genes will always translate into a person developing the disease. Prior to getting any genetic testing we strongly encourage our patients to consult with a genetic counselor. Many IPF programs are actively studying families affected by IPF.
Please read the article about genetics of IPF for more information. Patients that are identified with early disease may be candidates to begin treatment with OFEV or Esbriet to slow the progression of their disease.